Macular degeneration information
What is macular degeneration?
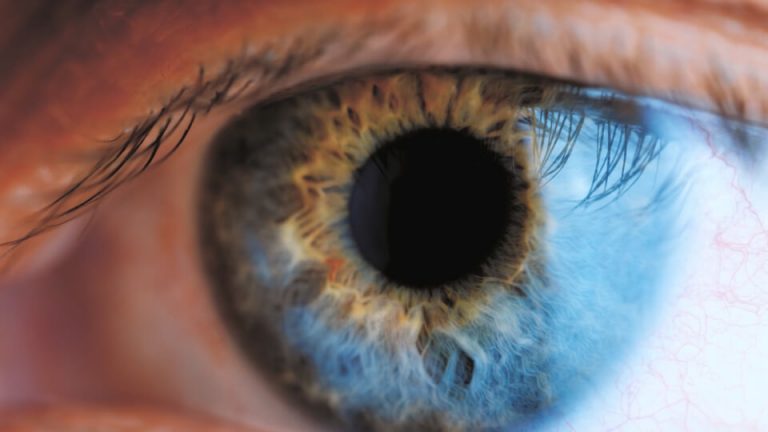
The macula is a small area on the back of the retina that is responsible for the fine detailed or central part of your vision. This provides vision which is important for reading, driving, recognising faces and doing most other visual tasks. In some people this area can wear out or degenerate. This can cause a loss of central vision, as outlined in the video above. The peripheral vision is usually not affected.
How common is macular degeneration?
Macular degeneration is common. It effects about 10% of people over 55 years of age. Not everyone will be affected by macular degeneration to the same extent. Over 75 years of age, 1 to 2% of people develop significant macular degeneration, with loss of vision. As a result, a common term for macular degeneration is age-related macular degeneration (AMD).
What causes macular degeneration?
The exact cause is unknown, however, several processes contribute to macular degeneration. These include advancing age, ultraviolet exposure, smoking, diet, some medical conditions and genetic susceptibility. There are also types of macular degeneration that are congenital or inherited.
Macular degeneration types
AMD is usually divided into two types, the ‘dry’ and ‘wet’ form.
In the ‘dry’ form, multiple small yellow dots, called drusen, form at the macula. It is thought that drusen are an accumulation of the breakdown products of cells in the retina. An accumulation of drusen can affect the flow of nutrients to the light detecting cells in the retina, affecting the vision. In 10% of people with dry AMD, there can be a loss of cells in the retina called geographic atrophy, which can lead to an advanced form of central visual loss.
In the ‘wet’ form, abnormal blood vessels grow from behind the retina. These blood vessels can bleed or leak fluid. This can cause a gradual or sometimes sudden significant decrease in central vision. The blood and fluid prevent the normal function of the retina, and can cause a scar to form, permanently damaging the central vision.
Dry AMD
Wet AMD
Macular degeneration diagnosis
How is AMD diagnosed?
Once AMD advances it can affect your vision and you will start to have symptoms of a central blur, distortion, or a loss of central vision.
Your ophthalmologist at Northpoint Eye Care will undertake a comprehensive examination of your eye to determine if AMD is the main cause of your visual problem. This will include visual acuity testing, intraocular pressure testing, slit lamp examination, and assessment of the health of the retina, particularly the macula, including detailed photographs.
The main method for imaging the macular is called optical coherence tomography (OCT). This is a non-invasive scan that gives a highly detailed cross-sectional image to the retina. The state-of-the-art OCT at Northpoint Eye Care can also give details of the blood vessels (angiography).
Some cases will require fluorescein angiography. This is where a special dye is injected into a blood vessel in your arm, so that photographs can be taken to highlight areas of abnormal blood vessels. It can be very useful in determining unusual cases of macula degeneration.
Macular degeneration treatment
Once AMD advances it can affect your vision
• Early detection
• Diet
• Quit smoking
• Intravitreal injections
• Low vision aids
• Collaboration
Early detection
Early treatment for wet AMD is critical. Anyone suffering from symptoms of central visual blur or distortion, or loss of central vision needs to present an ophthalmologist at Northpoint Eye Care soon as possible. Most people already diagnosed with macular degeneration should regularly check their vision using the Amsler grid.
Diet
Treatment of macular degeneration, both wet and dry forms can benefit from a healthy diet including lots of green leafy vegetables, fruit, nuts, fish and fish oils. There are certain vitamin and mineral supplements that are available. These will benefit some people as found in the Age Related Eye Disease Study (AREDS). This study found supplements of vitamin D, vitamin C, zinc, copper and carotenoids (lutein and zeaxanthin), may help to prevent vision loss in some people. If you have a healthy diet the supplements may not be required.
Quit smoking
Smoking is a significant risk factor for AMD. Smoking increases the risk of wet AMD by six times. We strongly advise you not to smoke, and encourage you to seek the help of your general practitioner to quit smoking. The Quitline national phone number is 13 78 48.
Intravitreal therapy
Treatment is aimed at preventing the build-up of an abnormal chemical called Vascular Endothelial Growth Factor (VEGF). Anti-VEGF drugs bind to VEGF and cause regression of the new blood vessels, and a reduction in the blood and fluid at the macular. In most people of this will also improve vision.
Anti-VEGF medications are given via an injection into the eye called an intravitreal injection. This sounds and looks dramatic, however, most people tolerate this very well. Treatment is given initially every month, and then the frequency is reduced according on the response to the medication. Most patients require ongoing treatment to maintain their vision.
Low vision aids
Low vision aids are various items that can assist if you develop severe central vision loss from AMD. There are also organisations that provide support and information to patients. See the links tab for useful links and or click for here for information about low vision aids.
Collaboration
Your general practitioner is invaluable in treating your AMD, especially counselling you on this significant change to your life and optimising your other medical conditions. Your optometrist is also invaluable in providing screening, prompt diagnosis and communication with your ophthalmologist when needed, and optimising your vision with spectacles or low vision aids. Follow the links tab for valuable information and resources.
Intravitreal injection process
Intravitreal injection can be a daunting procedure. We have provided a comprehensive booklet on the intravitreal injection process. This covers what happens before your procedure, on the day of your procedure and after your procedure. The answers to frequently asked questions are provided.
This information has been provided to guide you through the procedure process. If you have any questions please feel free to ask, we value that you feel comfortable and well informed about your procedure. Follow the link below for FAQs about the procedure.
NORTH LAKES DAY HOSPITAL
- 7 Endeavour Boulevard, North Lakes Qld 4509
- Tel: 07 3833 6755
- Fax: 07 3491 3614

Links
Share:
E-BOOKS